Continuous Glucose Monitoring: Going Off-Label
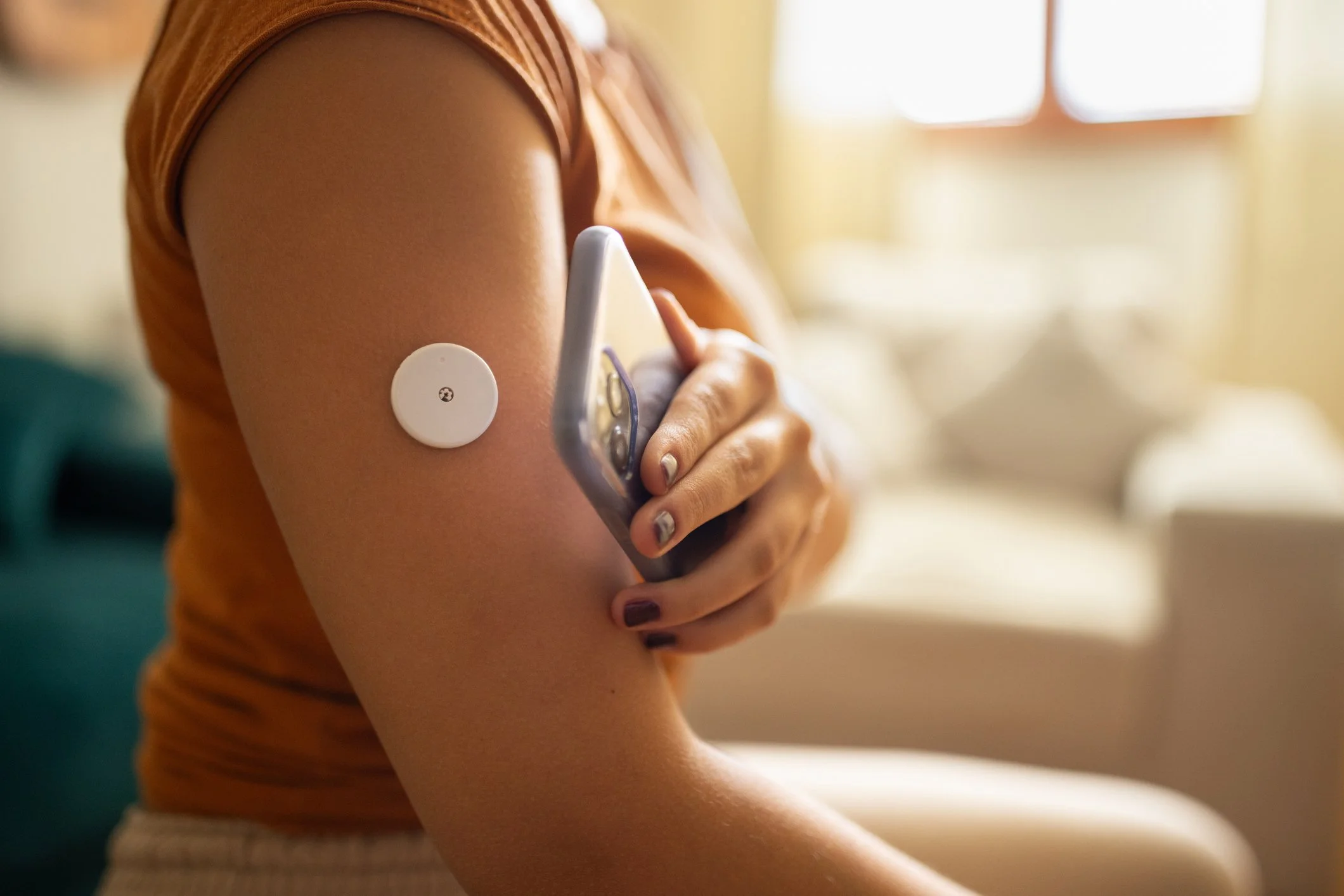
Continuous Glucose Monitor in action
A continuous glucose monitor (CGM) is a small patch worn on the back of the upper arm. It stays in place for about two weeks and measures glucose continuously. The data is transmitted to a phone or reader and updates every few minutes. You see your glucose level and a graph showing where it has been over time.
CGMs were developed for people with type 1 diabetes. Because this condition is life threatening, patients historically relied on repeated fingerstick glucose checks each day. Thankfully, continuous monitoring replaced that system.
The technology has since expanded to people with type 2 diabetes and others interested in understanding glucose patterns. Unfortunately, health insurance companies are generally more concerned with keeping people alive than with improving quality of life, so coverage often ends with type 1 diabetes. At the same time, the market for these devices has expanded enough that affordable out-of-pocket options are now available.
What a CGM shows is not just a glucose number, but timing. How quickly glucose rises after meals. How long it stays elevated. How efficiently it returns to baseline. This information is useful in cases of early metabolic dysfunction, reactive hypoglycemia, disrupted sleep, and unexplained fatigue. CGMs can also show how stress, pain, illness, and daily routines affect glucose regulation.
The downsides are minimal. The sensor is small. There is no medication involved. The primary barrier remains access.
If you have been told your labs are normal but your experience does not feel normal, a CGM may help explain the disconnect.